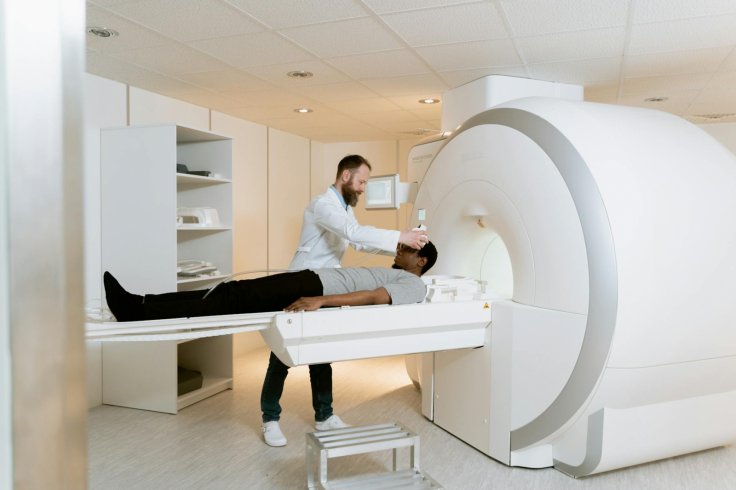
Researchers are using magnetic resonance imaging to quantify fat deposits in the pancreas of children and teenagers with obesity. The findings link elevated pancreatic fat to measurable increases in cardiometabolic risk. The work is reframing how clinicians think about obesity-related organ damage in young patients.
For most of the past decade, fatty liver disease dominated the conversation around pediatric obesity and metabolic health. The pancreas received comparatively little attention, in part because measuring fat accumulation in that organ without surgery or biopsy was technically difficult. MRI-based techniques have changed that calculus.
Peer-reviewed research published on the National Institutes of Health's PubMed Central confirms that free-breathing MRI protocols can now quantify pancreatic fat content in children and investigate how that fat is distributed across different regions of the organ, a property researchers call spatial heterogeneity.
A separate quantitative MRI method uses a metric called proton-density fat fraction (P-PDFF), a measure of the proportion of fat signal relative to total tissue signal, to assess pancreatic steatosis, or abnormal fat accumulation in the pancreas. Research published on ResearchGate found that P-PDFF readings are significantly associated with obesity in pediatric patients, establishing the measurement as a viable tool for clinical assessment in younger populations.
Reproducibility has also been confirmed: a study indexed on PubMed Central reported that MRI measurements of both liver and pancreatic steatosis show high reproducibility in adolescents with obesity and metabolic dysfunction-associated steatotic liver disease (MASLD), a condition marked by liver fat accumulation linked to metabolic dysfunction rather than alcohol use.
Pancreatic Fat and Cardiovascular Risk in Obese Adolescents
The clinical stakes extend well beyond the pancreas itself. Imaging-based research published on ResearchGate found that pancreatic steatosis in adolescents with obesity is associated with insulin resistance and subclinical vascular changes, meaning detectable damage to blood vessels that has not yet produced outward symptoms. Insulin resistance, in which the body's cells respond inadequately to insulin and blood glucose regulation deteriorates, is a primary precursor to type 2 diabetes.
Also Read: Trump Sets Two-Three-Week Deadline for US Military Exit From Iran
Research published in PubMed went further, finding that pancreatic steatosis shows stronger associations with cardiovascular disease markers than liver steatosis in obese adolescents.
That finding carries weight because liver fat, specifically non-alcoholic fatty liver disease, has long been the benchmark organ-level risk indicator in obese youth. Reporting from Mirage News and Bioengineer.org corroborates the link, noting that higher pancreatic fat content in children and adolescents with obesity is associated with increased heart and metabolic risk factors.
"Fatty pancreas is emerging as a major concern in Type 2 diabetes patients," with strong associations to abnormal glucose metabolism, according to expert commentary reported by The Health Site.
The downstream trajectory is supported by a study indexed on PubMed, which estimated that over half of adults with type 2 diabetes have fatty pancreas disease, representing what researchers described as a major unrecognized metabolic burden.
Childhood Obesity Scale and the Long-Term Pipeline to Adult Disease
The public health arithmetic behind these findings is difficult to ignore. India alone has approximately 41 million children with a high body mass index, ranking second globally, with 14 million of those children living with obesity, according to reporting by the Times of India.
Those figures have not been independently confirmed by a second source in the available research packages, but they reflect the scale of the population potentially affected by the pancreatic fat findings described above.
Obesity in childhood does not resolve automatically with age in numerous instances. Metabolism, the suite of biochemical processes the body uses to convert food into energy, begins developing before birth and shapes long-term health trajectories throughout life, according to research from the University of Alabama at Birmingham.
Fat that accumulates in the pancreas during childhood may therefore establish risk pathways that persist into adulthood, a concern that gives the MRI-based measurement work additional urgency.
Imaging studies are now being used across research centers to measure pancreatic fat content directly in children and teens, according to News Medical. The practical implication is that clinicians may eventually have a non-invasive, reproducible tool to screen for pancreatic steatosis in pediatric obesity cases before symptoms develop, much as ultrasound and MRI are currently used to monitor liver fat in the same patient populations.
The body of imaging research does carry limitations. Many of the studies involve relatively small cohorts drawn from clinical populations, meaning children already being treated for obesity or metabolic conditions.
Whether the pancreatic fat associations hold across broader, more diverse pediatric populations is a question the existing literature has not fully answered. Longitudinal studies tracking the same children from diagnosis through adulthood would be needed to confirm whether elevated childhood pancreatic fat fractions directly predict type 2 diabetes or cardiovascular disease in later life.
What the current evidence does establish is that the pancreas in obese children accumulates fat at measurable levels, that MRI can detect and quantify that fat reliably, and that higher fat fractions correlate with markers of heart and metabolic dysfunction that clinicians already treat as serious risk indicators in adult populations.
Disclaimer: This article was produced with the assistance of artificial intelligence.









