More than 415 million people are estimated to be suffering from diabetes across the globe. Until today, the most common treatment for the disease has been to either manage the disease with a carefully controlled diet and regular insulin shots, if required.
However, in a huge breakthrough for medical science, a team of researchers might have finally discovered the cure to the disease with some help from some diabetic lab mice.
Human stem cell strategy tested on diabetic mice
A team of researchers at the Washington University School of Medicine in St Louis successfully managed to convert human stem cells into ones capable of producing insulin, which helps to control the blood sugar level in the human body.
The researchers then used the insulin-producing cells to control blood sugar levels in diabetic mice and the results were more than impressive. Jeffrey R Millman, assistant professor at Washington University, who led the team, said their four-legged subjects suffered from severe diabetes with blood sugar levels of more than 500 mg per decilitre of blood, levels that could easily kill a human.
After giving the mice the insulin-producing stem cells, it didn't take longer than two weeks for their blood glucose levels to return to normal and "functionally cured" the mice of the disease for up to nine months.
Builds on earlier research
The new study builds on previous research, in which researchers successfully figured out a way to create these insulin-secreting cells using human stem cells. However, their effectiveness was not proven until now. One issue that cropped up was when converting the stem cells into another type of cell, there are always mistakes and random cells (off-target cells as researchers call it) are added to the mix along with insulin-producing ones. While these cells are harmless, they don't really help the cause either.
"The more off-target cells you get, the less therapeutically relevant cells you have," Millman said. "You need about a billion beta cells to cure a person of diabetes. But if a quarter of the cells you make are actually liver cells or other pancreas cells, instead of needing a billion cells, you'll need 1.25 billion cells."
When can it be tested on humans?
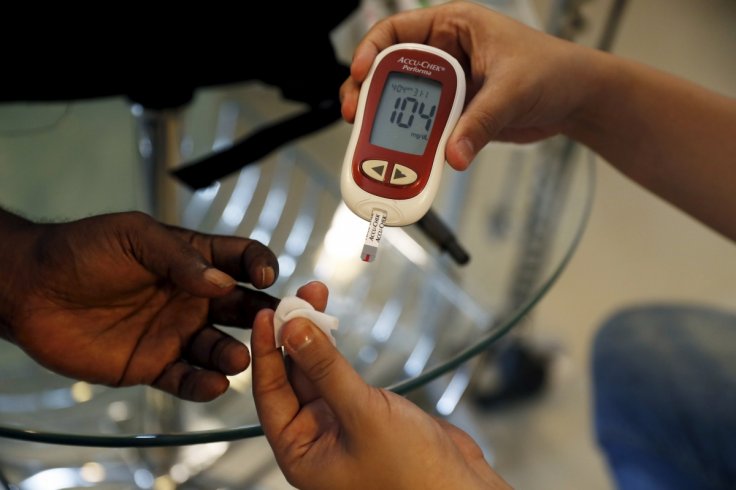
That said, the new research is more on-target and not only improves the effectiveness of the treatment but also maximizes the number of insulin-producing cells. While the experiment has been successful in lab mice, it will be a long time before it can be tested on human subjects.
The team plans to continue testing the cells on larger animals, and over longer time periods, with their sights set on human clinical trials in the future as researchers aim to eventually find an automated way to produce enough cells that allow humans to control their diabetes on their own one day.









