Since the beginning of the new Coronavirus pandemic, scientists and healthcare experts have faced an unprecedented task. Many have developed new tools to help with the early and efficient detection of the virus.
In the early days of the pandemic, with not every patient showing similar symptoms, doctors turned to chest X-rays and chest CTs (computed tomography) to understand the severity of the COVID-19. But reading chest X-rays to differentiate COVID-19 and other thoracic diseases is time-consuming. However, a group of researchers has developed an artificial intelligence tool to do just that.
The AI tool named DeepCOVID-XR, developed by researchers from the Northwestern University in Illinois, the U.S., can read chest X-ray images to detect COVID-19 more accurately and faster than thoracic radiologists. According to the research data published in the journal Radiology, the tool was put to the test and could detect the disease with 83 percent accuracy, scanning through 2,214 images.
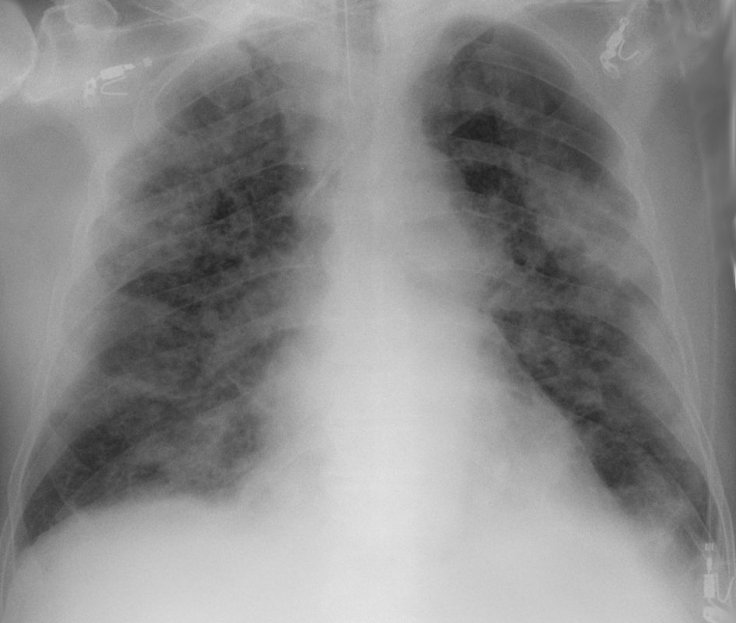
DeepCOVID-XR
As a COVID-19 test can take from hours to days to come, doctors can check chest X-rays and start treatment. The other advantage is that by screening chest X-rays, doctors can determine whether a patient needs to be isolated promptly. It would help in stopping the spread in the emergency facilities. So far, nearly 238,000 doctors have been exposed to the virus and 841 of them have passed away.
"It could take hours or days to receive results from a COVID-19 test. AI doesn't confirm whether or not someone has the virus. But if we can flag a patient with this algorithm, we could speed up triage before the test results come back," Dr Ramsey Wehbe, who was the other main author of the study, said in a press statement.
The AI model was trained with 17,002 chest X-ray images from the Northwestern Memorial Healthcare System sites with 5,445 of them from COVID-19 patients. The researchers then put DeepCOVID-XR to test with 300 chest X-rays from Lake Forest Hospital and compared the results with the interpretation of experienced cardiothoracic radiologists who spent between 2.5 to 3.5 hours to analyze. Researchers found that the AI tool could give results in only 18 minutes.
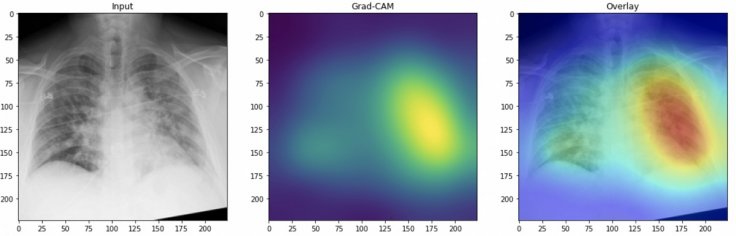
Not A Test Replacement
However, the tool is not meant as a replacement for a COVID-19 test. It is meant to flag an individual as a potential carrier of the virus. The other senior author of the study and an AI expert, Dr Aggelos Katsaggelos, said that while the tool was aimed at speeding up the process while waiting for the test results to be back.
"We are not aiming to replace actual testing. X-rays are routine, safe and inexpensive. It would take seconds for our system to screen a patient and determine if that patient needs to be isolated," he said.
The tool also has some limitations. Not all chest X-rays from COVID-19 patients show signs of the infection, especially in the early stages. Researchers found that only up to 56 percent of symptomatic patients show signs of infection in the early stage as the virus takes time for the virus to affect the lungs. Hence, the AI tool would not be able to detect signs of the virus from the X-ray images. Furthermore, many chest X-rays are non-specific as other diseases could also have an impact on the lungs, like other viral types of pneumonia.
But the researchers made the tool available for public use, hoping that hospitals and radiologists would continue using it. If the AI algorithm is trained with new data, it would get better and could be used in clinical settings in the future.
"We feel that this algorithm has the potential to benefit healthcare systems in mitigating unnecessary exposure to the virus by serving as an automated tool to rapidly flag patients with suspicious chest imaging for isolation and further testing," the authors said in the conclusion.









