Pancreatic cancer is the fourth leading cause of cancer deaths in people. It has one of the lowest survival rates and the life-expectancy post-diagnosis is one of the lowest among all forms of cancers. Therefore, tracing its development back in time can help in understanding how cancerous cells with specific mutations interact and invade, and enable better identification and treatment. However, how can one go back in time to study this? What will they find?
The researchers from Purdue University engineered a 'time machine' to understand the disease better and found that it is more unpredictable than known. When cancer cells grow together, they promote each other's growth, the researchers found.
Other than the discoveries made during the publication of the paper, that provided new insights into the evolution of the disease, the researchers have found drug resistance in types of cancer cells arising from two-drug sensitive ones.
What is the 'time machine'?
Made out of collagen, it is a hollow tube designed to mimic the microanatomy of pancreatic ducts realistically. Through the injection of cancer cells into the artificially created duct's microfluidic channels, the scientists can study the behaviour of cancer cells over a period of time by using the setup as a model.
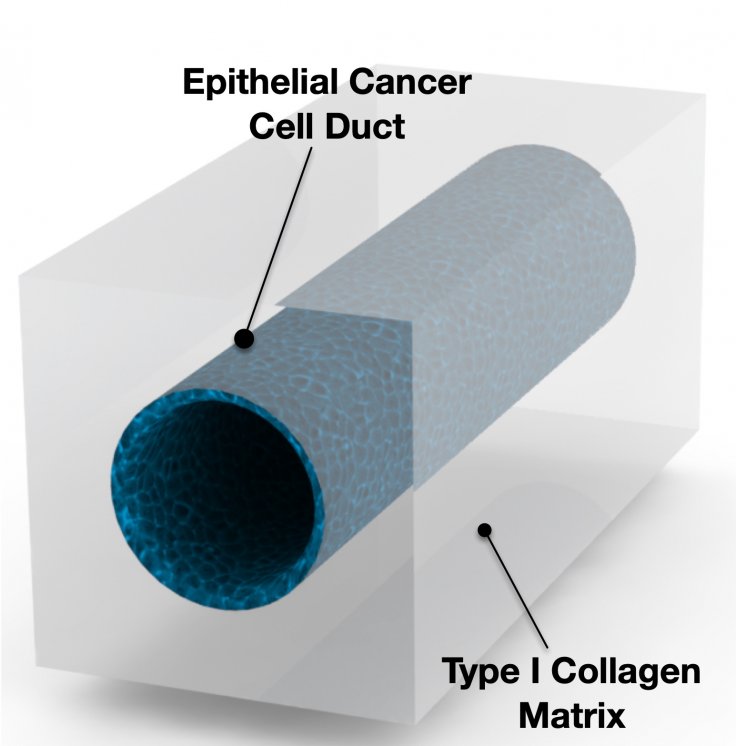
In a patient with pancreatic cancer, it generally takes nearly two decades for the disease to develop. An animal model also takes months to exhibit significant progress in cancer. However, the 'time machine' pancreatic cancer tumour model expedites the development of cancer to only two weeks. "We can observe what happens over a long period of time. This helps us to see trends that we wouldn't normally see," said Bumsoo Han, co-author of the study and a professor of mechanical engineering at Purdue University.
What makes the model so fast?
What makes this tumour model so fast is that the researchers can introduce cell lines from patients or animal models into the 'time machine' without waiting for genetic mutations to occur. The realistic layout of the model permits scientists to recreate mutations similar to what arises within the human body.
Going 'back in time' to make a concerning find
Using a mouse model, the researchers cultivated the pancreatic cancer cell line. The cell line was then loaded into the microfluidic channels within the artificial pancreatic duct. Once within the ducts, the cell lines began multiplying. In order to go 'back in time', the researchers simply rewinded the recordings made by the imaging equipment from the side of the life-like artificial ducts.
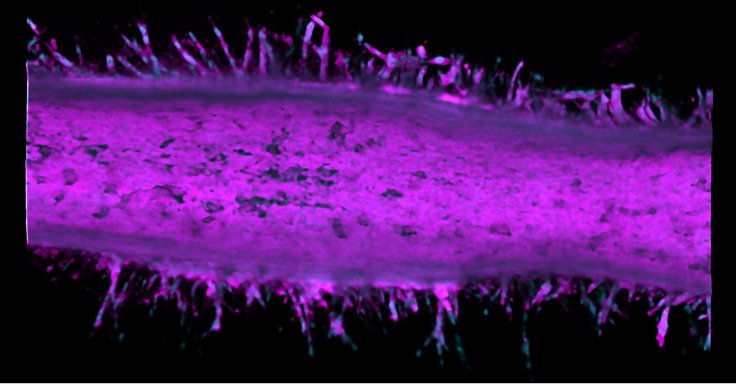
The researchers found that two different types of cancer cells fused into the device. After this, the cells became increasingly invasive and began sprouting from the ducts to form tumours.
What makes the artificial model so realistic?
The shape, say the researchers. Unlike a petridish, which is flat and limits certain aspects of development, the 'time machine' is not bound by it. "The curvature of the pancreatic duct affects the behaviour of cells. We could culture these cancer cells on a petri dish, but because the dish is flat, we wouldn't see the same behaviour," pointed out Han.
Potential to serve as a tool for drug discovery
Technically, cancer is a group of diseases. In the case of pancreatic cancer, there are four key driver mutations involved. Therefore, the scientists intend to study how each mutation of pancreatic cancer interact with each other. Furthermore, the tumour model can be employed as a pre-screening tool that can aid in the discovery of new drug targets for improved drugs, suggest the authors.
Pancreatic cancer
The pancreas is an organ that is an integral part of the digestive and endocrine system. When cancer develops in the pancreas, excessively dividing cells grow into tumours instead of healthy pancreatic tissue. The most common form of cancer in the pancreas—Pancreatic ductal adenocarcinoma (PDAC) —originates in the cells that form the lining of the ducts that carry digestive juices of enzymes from the pancreas.
According to the World Cancer Research Fund, 460,000 new cases of pancreatic cancer were diagnosed worldwide in 2018, with Hungary reporting the highest rate. The disease can be set off due to genetic factors or lifestyle factors such as smoking, alcohol consumption and obesity. Depending on the nature and rate of growth, it can be treated using methods such as surgery, chemotherapy and radiation therapy.









