Doctors have to deal with much more than the usual fight with death to save their patients. Often, they come across a moral dilemma which leaves them unable to decide the best course of action for the greater good.
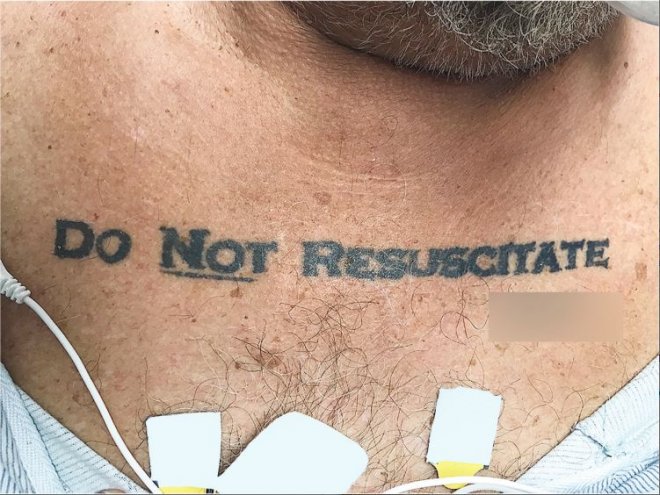
Such an incident happened at a University of Miami hospital when an unconscious patient was brought in with a tattoo across his chest which read "Do Not Resuscitate", followed by his signature.
The 70-year-old man was admitted to the hospital by paramedics who had found him inebriated and unresponsive. The man had a "history of obstructive pulmonary disease, diabetes mellitus and atrial fibrillation."
The tattoo on the man's chest put the doctors in a moral dilemma as to how to proceed with his treatment. As tattoos are not legally binding and authorised paperwork is needed for DNR approval, the doctors waited for several hours to make a decision.
The patient did not have any identification on him and the social work department was unable to contact his family. The doctors waited for the man to gain consciousness so they could discuss the next course of treatment, during which time they treated the elderly patient with antibiotics, vasopressors and intravenous fluids. However, when the man did not gain consciousness, an ethics consultation was requested.
"We initially decided not to honour the tattoo, invoking the principle of not choosing an irreversible path when faced with uncertainty. This decision left us conflicted owing to the patient's extraordinary effort to make his presumed advance directive known...", says the case study in The New England Journal of Medicine.
The ethics consultant advised the doctors to honour the patient's wishes, arguing that the "law is sometimes not nimble enough to support patient-centered care and respect for patients' best interests."
Following this, a DNR order was written and the patient was not subjected to any more life-saving efforts. The social work department soon found his DNR order approved by the Florida Department of Health, which supported their decision as it was consistent with the tattoo. The man's health worsened through the night and he passed away without any cardiopulmonary respiration efforts or advanced airway management.
As tattoos are not reliable or legal sources of information and may also represent past regret, the doctors were very confused about their course of action. However, the case study mentions that it "neither supports nor opposes the use of tattoos to express end-of-life wishes when the person is incapacitated."









