While Europe has been declared the new epicentre of the COVID-19 pandemic by the WHO, it is important to remember that the outbreak began in China. Beginning at the accepted epicentre —Wuhan, in Hubei province — the virus rapidly spread across the country affecting over 81,000 people. Not only did it pose an administrative challenge, it also tested the capabilities of China's healthcare system, prompting the adoption of innovations and improvisations.
In several cases, surgical intervention was required to save the lives of confirmed or suspected coronavirus patients. In a newly published letter to the editor, two Chinese doctors — Xianjie Wen and Yiqun Li, both from hospitals in Guangdong Province — offered recommendations on the right procedure of administering anaesthesia and the surgical precautions to be adopted while operating on suspected or confirmed COVID-19 cases
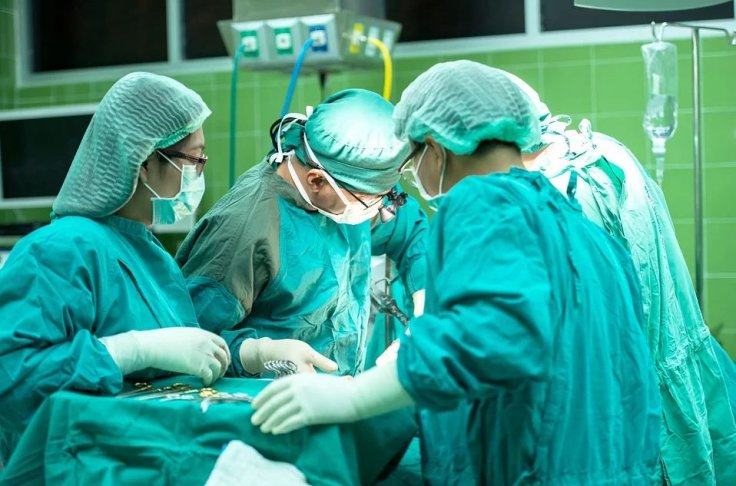
What did doctors in China do before operating COVID-19 patients?
All candidates for surgery were subjected to epidemiologic investigation and pre-examination in order to spot any missed diagnosis. Their travel history was looked into with a special focus on travel to Wuhan or interactions with those who had travelled to the epidemic area within 14 days.
Next, all the surgical patients were asked to submit to temperature reading, laboratory examination, and chest computed tomography scan. Following this, they were operated upon.
Prioritization and preparation of the operation theatre
In the letter, the doctors called for the cancellation of elective surgical procedures. Dr Bruce Aylward, the Assistant Director-General of WHO, during an interview, had pointed out that hospitals in China had put elective surgeries on hold to focus their efforts and resources towards the treatment for COVID-19. In the event of unavoidable emergency surgery, the authors impress upon the use of negative pressure operating rooms.
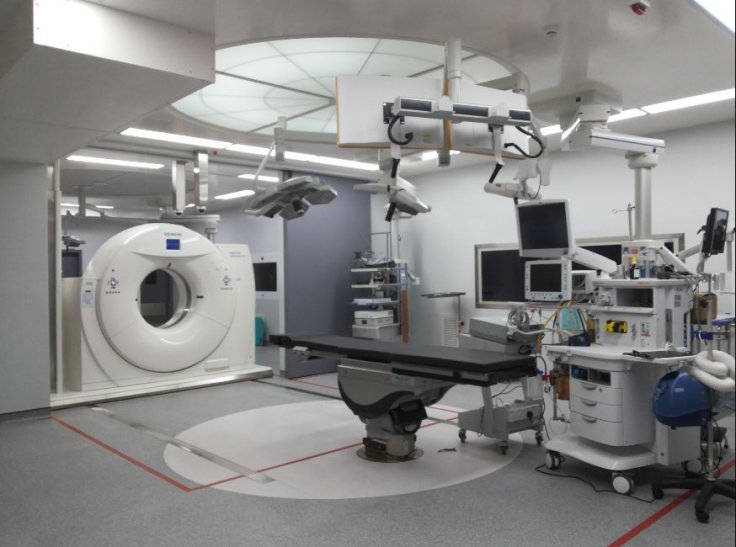
A negative pressure room is one where a ventilation system removes more exhaust air from entering the room. Typically, such rooms are used in the isolation wards of hospitals and medical centres especially, as part of quarantine of contagious diseases such as chickenpox and tuberculosis. Negative pressure operating rooms are used when surgeries have to be performed on patients who have communicable conditions.
Safety of the anesthesiologist
Emphasizing on the safety measures to be adopted during the administration of anaesthesia, the doctors stressed that the special assignment of drugs, anaesthetic equipment and appliances solely for such individual cases is paramount. While operating on such patients, monitoring anaesthesia or general anaesthesia must be adopted they added.
Most of all, they highlighted that the safety of the attending anesthesiologists is equally important. "Anesthesiologists should be protected according to the three-level protection requirements," the doctors wrote. Protection requirement refers to a particular type of surgical gowning method used depending on the scale of surgery. Three-level protection is employed for a wide range of surgical procedures and offers moderate fluid protection.
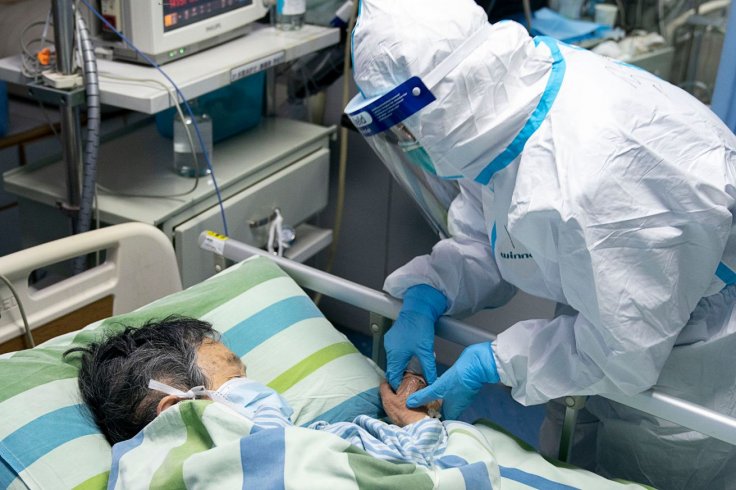
Employing the right procedure of administering anaesthesia
Cough droplets are considered as one of the primary sources of transmission of the highly virulent infection. Therefore, the doctors recommend the use of "fast induction" of anaesthesia —a technique also known as Rapid sequence induction (RSI) — in combination with muscle relaxants to prevent the patient from coughing. The authors also provided a specific order in which the anaesthetic agents must be administered — muscle relaxation drugs, intravenous general anaesthetic and opioids to avoid cough.
They added that before the patient loses consciousness, mask pressurization ventilation should be avoided. "The operating room must be disinfected after the operation. The relevant person contact with SARS-CoV-2 infectious pneumonia should be isolated and observed for 14 days," they wrote, underlining the importance of post-operative precautions.
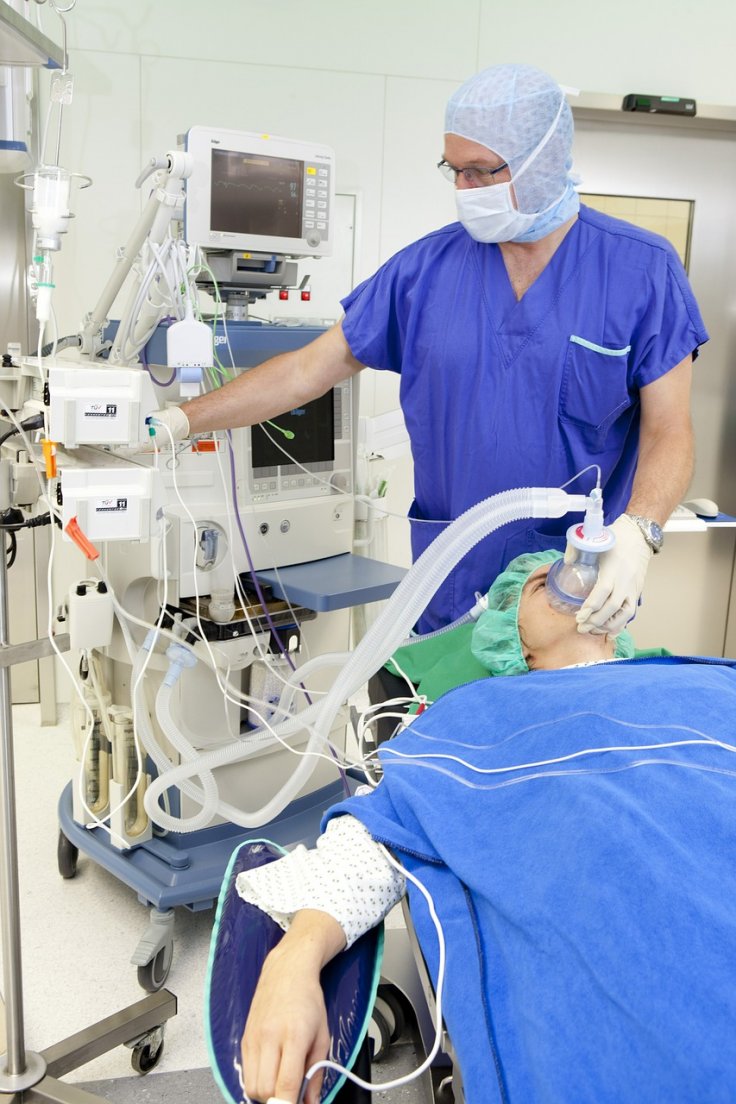
Mechanical ventilation procedures
During operations, mechanical ventilators are used to help the patient breathe. Also, anaesthesia maintenance is carried out during surgical procedures as the effects of the anaesthetic agents wear out after a fixed duration. This is where special care must be taken the physicians placed emphasis on. "During anaesthesia maintenance, a small tidal volume of lung-protective ventilation strategy should be adopted to reduce ventilator-related lung injury," they instructed.
Providing more technical intricacies they said, "Tidal volume is 4–8 mL/kg ideal body weight, inspiratory plateau pressure is less than 30 cm H2O, and PEEP level is less than 8 cm H2O and recruitment manoeuvres per 30 min. Ventilation parameters were adjusted by blood gas analysis and PetCO2 during the operation."









