We now know that COVID-19 is only mild to moderate for 80% of laboratory confirmed patients and about 6.1% patients get critical (respiratory failure, septic shock, and/or multiple organ dysfunction/failure), according to the joint WHO - China mission. Clearly, those who are in the critical stage are prone to death, most of them are aged more than 60, especially those with underlying conditions such as hypertension, diabetes, cardiovascular disease, chronic respiratory disease and cancer.
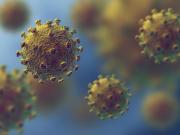
With 110,297 confirmed cases of COVID-19 and 3,840 deaths, more than 62,000 have recovered, as of Monday, March 9. The coronavirus is majorly transmitted through droplets and fomites via nose, mouth and eyes, during close unprotected contact between the infected and a normal person.
The majority consists of mild cases, and hence told ,Tom Inglesby, director of the Johns Hopkins Center for Health Security and an expert in pandemics and public health preparedness in a statement, "The more we diagnose mild cases, the more that will drive down the overall case mortality rate." The challenge is to identify mild cases, while severe cases are identified easily owing to symptoms.
The Tipping Point
In the case of the 6% who get critical, there is a "tipping point, where everything is going downhill and, at some point, you can't get it back," David Morens told news agency Bloomberg. Morens is the senior scientific adviser to the director of the National Institute of Allergy and Infectious Diseases, US.
The virus, at first, usually infects the nose. If it stays there, that's not fatal, but dangerous once it hits the lungs. Once it is down the windpipe to the peripheral branches of the respiratory tree and lung tissue, it take the patient to the critical stage (pneumonia-causing damage), explains Jeffery K. Taubenberger to Bloomberg who is the head of the viral pathogenesis and evolution section of the National Institute of Allergy and Infectious Diseases in Bethesda, Maryland
Normally, if white blood cells consume pathogens and help to heal damaged tissue as a body's immediate response, it can clear the infection, he adds. But damage would result in loss of protective mucus-producing cells as well as the tiny hairs, or cilia, that sweep dirt and respiratory secretions out of the lungs. "You have no ability to keep stuff out of the lower respiratory tract,"
You can't physically repair lungs
Secondary bacterial infections are a great threat, in addition to coronavirus, as they kill the respiratory tract stem cells that enable tissue to rejuvenate,Taubenberger said adding that lungs would starve vital organs of oxygen like the kidneys, liver, brain and heart. "You just can't physically repair your lungs," he adds.
This is a cascading action. "When you get a bad, overwhelming infection, everything starts to fall apart in a cascade," said David Morens. Those among the 6% are prone to experiencing this "tipping point".