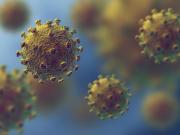
In the current coronavirus-altered world, venturing outdoors without a mask is nothing short of inviting trouble. This is because scientists across the world agree that droplets and mucous discharged during coughing and sneezing are one of the primary modes of transmission of the infection. However, an interesting question is that can other bodily fluids transmit COVID-19? Specifically, can tears transmit the disease?
A study published in the journal of the American Academy of Ophthalmology, suggests that transmission of the infection through tears is not likely. In the research conducted among COVID-19 patients in Singapore, no viral shedding was found in their tear samples. "The results from this study suggest that the risk of SARS-CoV-2 transmission through tears is low," the authors wrote.

The Hypothesis
The mode of transmission of COVID-19 is an aspect of the disease where research is ongoing. However, the transmission of infection through ocular fluids or tissue is contended upon. It is hypothesized that the virus can travel from the upper respiratory tract—where the infection develops—to the eye through the nasolacrimal system. The nasolacrimal system is the channel through which tears enter the nasal cavity from the external eye.
Analysing tears for the presence of coronavirus
Tear samples from 17 patients who were diagnosed with COVID-19 were collected for testing by the researchers. Beginning with the time when they exhibited symptoms until their complete recovery in approximately 20 days, the samples were collected regularly. What the doctors found was that during the course of the two-week period of the disease, no virus was detected in the tears, either in the viral culture or in the reverse transcription-polymerase chain reaction (RT-PCR) test.
Nonetheless, an intriguing question remains. If the patients' tears showed no viral load, what would samples from their nasal cavities and throats reveal? The question is of importance because, as mentioned earlier, droplets are considered the primary mode of transmission.
Factoring this consideration, the scientists simultaneously gathered samples from the patients' noses and throats through swabs. Unlike tears samples, the viral load found in these samples was immense. Dr Ivan Seah, co-author of the study, expressed hope that these findings could inform other research directed towards the prevention of the virus' transmission through other crucial modes such as fecal-oral spread and droplets.
Absence of conjunctivitis a limitation
While the study offers insights into the potential modes of the diseases' transmission, it is not without limitations. The most prominent one being that none of the patients suffered from conjunctivitis. Several ophthalmological reports suggest that 1 to 3 percent of COVID-19 cases develop conjunctivitis as a symptom.
Of the 17 enrolled patients, 16 presented no ocular symptoms, and only one developed a conjunctival infection during their stay at the hospital. Also, as the patients were already distressed by the disease, the doctors did not collect conjunctival tissue samples in order to refrain from causing further discomfort.
Stressing on the difficulties associated with the study of eye-related symptoms, the authors wrote, "Studying patients with ocular symptoms can be difficult. In a study of 1,099 COVID-19 patients, only 0.8 percent developed conjunctival congestion." Other limitations included a small sample size and the difference in the laboratory testing methods between the two sample types.
Potential for further research
Despite not including patients afflicted with conjunctivitis, the researchers maintain that their results suggest a low risk of ocular transmission. However, they call for studies that consider the involvement of patients with ocular symptoms.
The authors mention that in the event of a conjunctival infection, cell death will occur due to immune reaction or virus-induced lysis. Viral material will be released into the tears upon cell death and can be detected through RT-PCR. As SARS-CoV-2 gains entry into cells using ACE2 receptors, the authors call for focused studies that can conclusively prove the presence of ACE2 in the conjunctival and corneal cells. They also add that future studies should take into consideration the link between serum viral load and viral shedding found in tears.