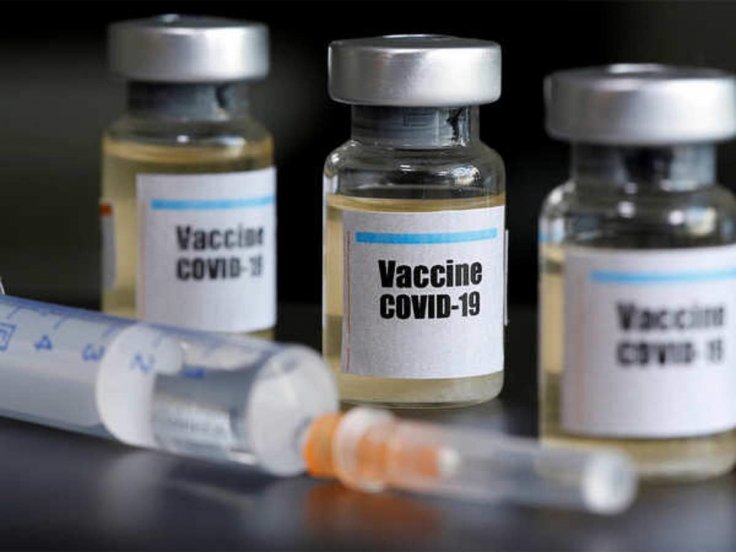
With China and Russia both approving their Coronavirus vaccine candidates for limited use amid the ongoing Phase III trials, health experts have raised concerns about their effectiveness.
Out of multiple vaccine candidates that China and Russia are developing, the ones made by CanSino Biologics and Gamaleya Institute have been approved for limited testing. However, both vaccines are based on the common cold virus or Adenovirus vectors that has been exposed to people already. Experts believe Adenovirus based vaccines will be less effective against COVID-19.
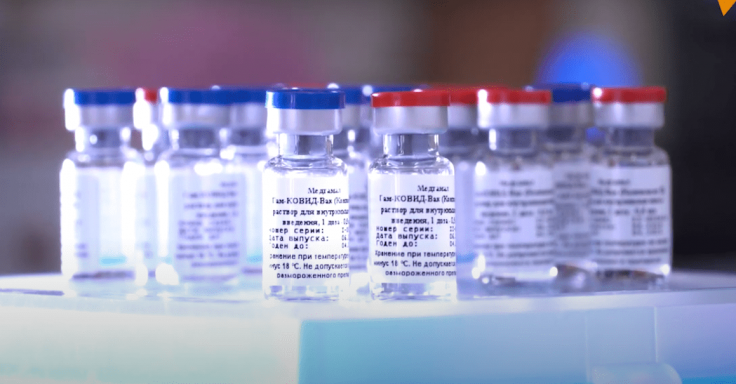
Sputnik V, Russia's COVID-19 vaccine was approved earlier this month (August 2020) will be given in two doses. The first dose is based on Adenovirus-26 (Ad-26) but the second one will be based on the type 5 Adenovirus. CanSino Bio's vaccine too followed the same path. The vaccine, which was given to China's military with limited approval, is also based on a modified version of Ad-5. The company is also in talks with other countries to get emergency approval although it has not been tested in a large scale.
Why Could It be Ineffective?
Adenovirus causes respiratory distress, pneumonia and fever, or common cold but over time, the human body has developed immunity against the virus. That's the reason scientists believe Ad-5 based COVID-19 vaccine may not be effective as the human immune response will target the Ad-5 vectors instead of attacking Coronavirus. That will make the vaccine less effective.
As per experts, about 40 percent of China and the U.S. population has high levels of antibodies due to previous exposure while in Africa, the number could be 80 percent. Hence, Johns Hopkins University's Anna Durbin, a vaccine researcher, believes that the Ad-5-based COVID-19 vaccine might not have 70 percent or above efficacy.
"The Ad-5 concerns me just because a lot of people have immunity. I'm not sure what their strategy is. It might have 40% percent," she told Reuters, adding that it could still provide a stop-gap immunity against COVID-19 "until something else comes along."
Dr Hildegund Ertl, Director of the Wistar Institute Vaccine Center in Philadelphia, said although it would help create an immune response in a lot of people who don't have antibodies, it will not be effective in the rest who already have them.
Popular Choice
Adenovirus has been a popular virus for vaccine research for other viruses. There are several types and subtypes for animals and humans. Researchers use harmless Ad-5 as vectors to transport genes from the target virus to cells to induce an immune response and fight the virus. For SARS-CoV-2, which causes COVID-19, the Ad-5 based vaccine will follow the same method.
However, despite the fears that it could be ineffective, many vaccine developers have chosen adenoviruses for their delivery mechanism. The leading vaccine candidate which is being developed by Oxford University and AstraZeneca is also based on adenovirus but of a different kind. They are using chimpanzee adenovirus for the COVID-19 vaccine to eliminate the risk of Ad-5 immunity.
Johnson & Johnson's COVID-19 vaccine candidate is also based on adenovirus, but on Ad26, a rare strain. Both Gamaleya and CanSino Bio have approved vaccines for Ebola that are based on Ad-5.
Potential Risks Including HIV
Experts also warn of potential risks the adenovirus-based vaccines might have. Dr Zhou Xing from Canada's McMaster University had worked with CanSino Bio's Ad-5 based vaccine for tuberculosis in 2011. He is concerned that high doses of the Ad-5 vector could cause fever which would scare a lot of people who are already skeptical about vaccines.
Xing also worries that high doses of the Ad5 vector in the CanSino vaccine could induce fever, further fueling vaccine skepticism. Some scientists are also concerned that Ad-5 based vaccine could make people susceptible to HIV (Human Immunodeficiency Virus).
Merck & Co conducted an Ad-5 based HIV vaccine trial in 2004 and found that people with pre-existing conditions became vulnerable to HIV. Even Dr Anthony Fauci, top infectious disease specialist from the U.S. in a 2015 paper titled, Toward an HIV Vaccine: A Scientific Journey, said, "vaccine-related immune activation might have led to increased susceptibility to infection."
Dr Larry Corey, who was a lead researcher on the Merck HIV vaccine trial and co-leader of the U.S. Coronavirus Vaccine Prevention Network, said he would be worried if Ad-5 based vaccines are given in countries with a high risk of HIV. The U.S. falls in the high-risk category.









